Understanding your body’s glucose response remains a critical component of any diabetes management plan, but can also serve as a valuable tool for anyone who wants to know the state of their metabolic health.
Tracking your glucose can allow you to discover irregularities in your body’s processing of glucose, learn what causes your glucose to spike, and whether your glucose levels fall into average ranges. This article will delve into the importance of tracking glucose and shine light on some of the metrics that may be most useful for you to track.
Why Is Tracking Glucose Important?
f you live with type 1 diabetes or type 2 diabetes, tracking glucose is a standard place to start the management of this chronic disease. However, tracking glucose isn’t just for diabetes care; it can be extremely beneficial for non-diabetic people who want to establish a baseline understanding of their body’s glucose regulation patterns for other health purposes.
Recent studies reveal that non-diabetics have larger fluctuations in their glucose levels1 than previously thought, and finding ways to stabilize glucose proves beneficial for health in many ways, such as:2
- Weight loss
- Weight maintenance
- Building muscle
- Consistent energy
- Optimal fueling strategy for peak athletic performance
- Lower and control inflammation
- High-functioning immune system
- Lower risk of chronic diseases such as heart disease and obesity
Instead of viewing glucose tracking as a reactive approach to ailments, consider it a viable way to protect your health and prevent avoidable diseases. Even if certain irregularities revealed in your blood sugar metrics don’t point to diabetes or metabolic disorders, they could still indicate other health issues.
{{mid-cta}}
What Are the Most Important Glucose Metrics to Track?
There are several metrics to measure glucose levels, but each provides a different insight into the bigger picture of metabolic health.
How to Measure Blood Glucose
Monitoring and measuring blood glucose is an essential place to start to determine the status of your metabolic health. Below are a few ways your healthcare provider could measure your glucose levels.
Glucose Tolerance Test
Often used in pregnancy, the oral glucose tolerance test (OGTT) requires drinking a specific amount of glucose and testing glucose at one, two, and sometimes hours after. If your test results exceed 200 mg/dL after two hours, you may be living with diabetes and need to speak with a medical professional about possible next steps.
Fasting Glucose Test
The fasting glucose test is administered after an individual fasts for at least eight hours. This is normally a blood test and measures the glucose in your blood rather than your urine. If you receive a test result showing your fasting blood glucose is below 100 mg/dl, you are considered non-diabetic.
Average (Mean) Blood Glucose Levels & Glycated Hemoglobin (HbA1c) Tests
If you have abnormal fasting glucose levels, your physician may order a glycated hemoglobin (HbA1c) test, one of the most indicative benchmark tools physicians currently use to understand, track, and manage blood glucose health. The HbA1c test is sometimes referred to as A1c.
This blood test measures a person’s blood glucose levels over a three-month period and is a diagnostic tool for prediabetes and diabetes.3 Through the results of this test, physicians may be able to determine your average (mean) blood glucose levels.
However, this test will not give you insight into why the changes in your HbA1c occurred. Studies have shown that HbA1c is not as accurate in non-diabetic populations compared to those living with diabetes, as HbA1c does not capture glucose variability information, which is an important measurement for both populations.4
Glycemic Variability
Glycemic variability, or swings in blood glucose levels, is an important metric to monitor. Remember that certain degrees of glucose variability, or fluctuation in glucose, is normal; this has to do with circadian rhythms, hormones, and the regulation of important bodily functions.
However, this could indicate complications when swings in glucose become abnormally radical, reaching dangerous peaks or lows, or vacillating between hyperglycemia and hypoglycemia.
CGM for Non-Diabetics: How Does it Work?
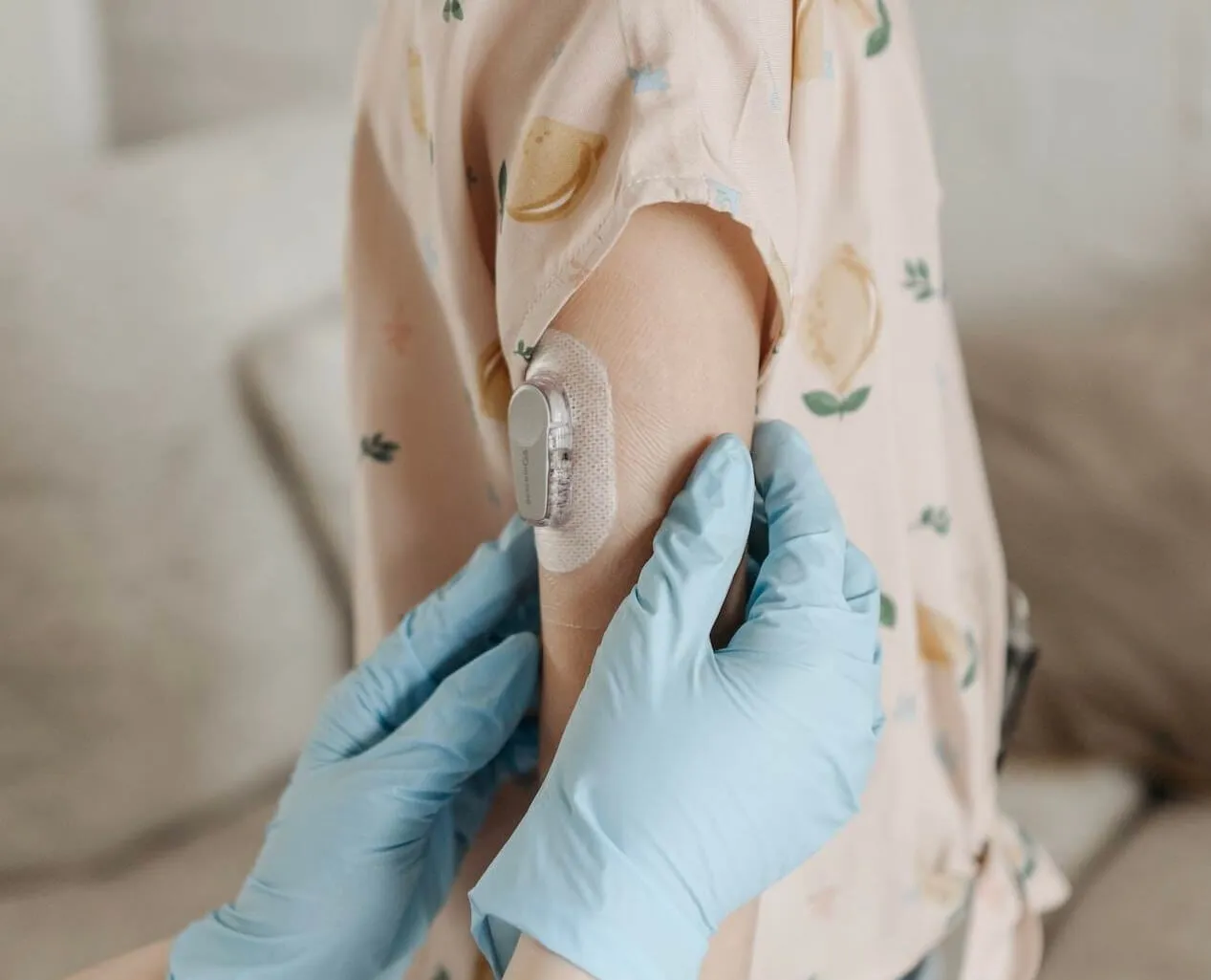
A CGM is a tiny wearable device that reads your glucose levels in real-time. It is attached to your body (usually worn on the upper arm or the stomach) and continually monitors how much glucose you have circulating in your body at any time without painful finger sticks. CGM devices have two parts: a sensor and a transmitter. The sensor is worn under your skin, and the transmitter sends results to a wearable device or cell phone. You keep the continuous glucose monitor on at all times, including in the shower, when getting your sweat on, and when you sleep.
The CGM sensors can stay in place between 10 and 14 days before they need to be replaced. The exact duration depends on the manufacturer, but you will be alerted when it’s time to replace the sensor. When taking it off, just peel off the adhesive like you would peel off a bandaid.
A CGM provides people with information about how their bodies manage blood sugar throughout the day in response to one’s daily activities. Food, sleep, exercise, and stress impact blood sugar differently, and wearing a CGM provides a new way to understand how your metabolism functions.
There are two main CGM manufacturers in the US: Dexcom and Abbott. The current models are the Dexcom G6 and Abbott Freestyle Libre.
Reasons for a Non-Diabetic to Use a CGM
Knowledge is power. So, why would a person who does not live with diabetes want to monitor their blood sugar? Reasons include:
- Detect earlier prediabetes
Glucose data could provide individuals with an in-depth look at underlying health conditions, like prediabetes, that normal screening would not have detected.
- Helps to use blood sugar levels to improve mental or physical performance
Knowing how dietary choices, stress, and sleep impact your body can lead to sustainable changes that can lead to a healthier lifestyle. Metabolic health varies for each individual, and knowing what directly impacts your body could influence your wellness goals and lead to numerous health benefits, including better sleep, choosing whole foods, and prioritizing stress relief techniques.
- More control over health
More information about your body can give you a sense of control over your health, even if you decide not to change your lifestyle.
How to Get a CGM for Non-Diabetics?
You will need a prescription from a healthcare provider to obtain a CGM. However, not all providers recommend using a CGM if you are not at risk for prediabetes or diabetes.
Another option is paying out-of-pocket for the device and purchasing it through a third-party company. Third-party companies include Levels Health, Nutrisense, and Signos.
Signos will work to obtain a prescription on your behalf and send you all the necessary materials to get started. Plus, you can access the Signos AI-driven app, real nutritionists, and a supportive Facebook group with other members. This support is essential as you start your journey and learn how to interpret the CGM data.
Why Individual Treatment Matters
Rather than one supremely important glucose metric, it’s most beneficial to keep an eye on multiple glucose metrics at once. This is why individualized treatment is crucial. The more data you can gather about your health, the more your physician can use it to evaluate what needs to be done to protect it. No matter what, one of the most crucial aspects of monitoring your glucose is ensuring your treatment plan is individualized. The most important glucose metric to track for one person may be different for another.
References
- https://pubmed.ncbi.nlm.nih.gov/20396998/
- https://care.diabetesjournals.org/content/28/12/2939
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5444503/
- https://pubmed-ncbi-nlm-nih-gov.laneproxy.stanford.edu/28699985/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2797987/



.svg)









.svg)
.svg)
.svg)
.svg)
.svg)
.svg)
.svg)
